UroLift Healthcare Team
![]()
What is the UroLift System?
The UroLift® System treatment is a revolutionary, minimally invasive approach to treating an enlarged prostate, or BPH, that lifts or holds the enlarged prostate tissue out of the way so it no longer blocks the urethra. There is no cutting, heating or removal of prostate tissue.
Clinical data has shown that the UroLift System treatment is safe and effective in relieving lower urinary tract symptoms due to BPH without compromising sexual function1,4. The goal of the UroLift System treatment is to relieve symptoms so you can get back to your life and resume your daily activities.
Most common side effects are light blood in the urine, some pain or discomfort when urinating, some increased urge to go and discomfort in the pelvis that typically resolve within two to four weeks after the procedure.
New Treatment Can Help Men With An Enlarged Prostate
An article by IUI Physician Dr. Joseph H. Williams
New Treatment Can Help Men With An Enlarged Prostate
For most urologists, the pesky prostate gland occupies most of our clinic day. The prostate gland in men is an organ that makes fluid for semen. It is positioned between the bladder and the urinary sphincter in the pelvis. The urethra, the tube that carries urine from the bladder down and out of the body, goes right through the middle of the prostate.
There are three main types of problems that occur with the prostate. The first involves prostate infections or painful prostate conditions. The second involves benign prostatic hyperplasia (BPH), or overgrowth of the prostate that occurs as men age beyond their 30s. The third category of prostate problems is prostate cancer. One of these categories of problems does not lead to a problem in another category. In other words, there is not a cause-effect relationship between having an enlarged prostate or an infected prostate and prostate cancer.
It is perfectly normal for a man’s prostate to enlarge. In fact, it is an expected part of aging. The prostate can enlarge or expand in size outward and/or inward. The patient can have a really big enlarged prostate and not have any urination difficulties or a patient can have a mildly enlarged prostate and need an operation. Everybody is different.
Seventy percent of men over age 60 have some symptoms of having an enlarged prostate. Because of the urethra being squeezed by the enlarged prostate, the bladder may have to work harder to get urine out during voiding. This can result in a weak or slowed urinary stream. Sometimes the bladder cannot empty because of the constriction. This may result in increased frequency of urination, both during the day and possibly while the patient is trying to sleep. Patients can have a sense of not completely emptying the bladder with BPH. There can be a delay in the start of urine flow once the patient is trying to urinate. The urine stream can start and stop if the bladder is trying to push urine through.
Treatment
If a man begins to have symptoms of having an enlarged prostate, we have several options in managing it. Historically, surgery was the only answer.
But in the early 1990s we developed two classes of medications that can help with BPH therapy. First, there was a pair of medications called the 5-ARIs. Finasteride and dutasteride actually over time shrink the prostate, as they change the hormonal mechanism by which the prostate continues to grow. A small percentage of men have sexual side effects from this medication. However, we have demonstrated that – with long-term use – they confer a 30 percent decrease in the incidence of prostate cancer developing. Together with alpha blocker medications that relax the prostate capsule and bladder neck, men can have significant improvements in their voiding parameters with medical therapy.
Sometimes this is not effective enough or the patient’s prostate requires a surgical option. Classically we performed removal of tissue to include the prostatic urethra and impinging prostate tissue using a scope with the patient under anesthesia. This is called Transurethral Resection of the Prostate, or TURP. In the early 1970s this was the most commonly performed surgery in the United States. Over time we have developed several other procedures whereby different energies, to include microwave heat, laser vaporization and now most recently steam pressure, to cause a similar defect. These procedures do not remove as much tissue as a TURP does. The TURP remains the gold standard and of all treatments patients who have had a TURP are from avoiding standpoint the happiest long term.
Ten to 15 percent of patients who have a TURP require other therapy at some point in their lives. With the lesser tissue removal procedures, more patients need something done at another point in their lives than with a TURP.
The new procedure
About 12 years ago, a group of engineers got together and tried to come up with a new way of approaching an enlarged prostate. Their brain child was approved by the FDA about five years ago. It is called the UroLift. With the UroLift procedure, we place small filaments of thread that are attached to anchors outside the prostate and on the inside of the prostatic urethra that open the prostatic urethra and can effect a significant amount of relief from BPH for men who have a mildly to moderately enlarged prostate. A really neat aspect of this device is that it can be done without any tissue removal and therefore the anesthesia requirements are less. Frequently we can do it with just local anesthesia and possibly sedation via an IV. It is therefore an outpatient surgery and can happen quite quickly with a very early recovery.
Patients ride home after the procedure and can do pretty much whatever they want the following day. For the first 2 to 4 weeks they can have a sense of urinary urgency and frequency, but this goes away once the prostate gets used to having tissue compressed.
One of the biggest differences between the tissue removal procedures and the UroLift is that the bladder neck, the dividing line between the bladder and the top of the prostate, is not touched. Men who have had surgery and some men who have alpha blocker medical therapy can have what is called retrograde ejaculation, where seminal fluid goes up into the bladder as opposed to out of the urethra with an orgasm. UroLift preserves this function, so a lot of men look upon the UroLift as a way to manage their early BPH symptoms without sexual side effects.
When the UroLift procedure first came out, there were concerns amongst urologists that the procedure would not last very long or there could be complications of having the inner filaments calcify with material. Over a five-year period of following patients who were initially involved in the FDA-approved trials five years ago, we have seen a very low complication risk and a very impressive set of data regarding durability of symptom improvement.
Again, a main point to catch here is that every man is different and every man’s anatomy is different. Every patient with BPH requires an evaluation and a tailoring for therapy to work on their specific problem. It is really great in the urologist’s office to have more and more tools to take care of this significant problem.
Find more information about an enlarged prostate at http://www.idurology.com/enlarged-prostate/
Advantages of the UroLift System:
- Rapid symptom relief, better than reported for medications2
- Risk profile better than reported for surgical procedures such as TURP3
- Preservation of sexual function1
- Return to normal activity in days not months
- Increased quality of life
- No ongoing BPH medications
- 19 clinical study publications; 4 years published clinical data4
How the UroLift works:
The UroLift System treatment is a straightforward procedure that is performed by a urologist. The urologist places tiny implants to hold the prostate lobes apart, like open curtains on a window, to relieve compression on the urethra. This allows urine to flow normally again. The UroLift System treatment can be done in the physician’s office under local anesthesia. Typically, patients return home the same day without a catheter.2
How the UroLift System Works
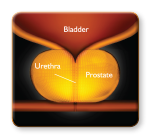 |
Enlarged Prostate: An enlarged prostate compresses on the urethra, making it difficult for urine to flow |
 |
Step 1: The UroLift Device is placed through the obstructed urethra to access the enlarged prostate. |
 |
Step 2: Small UroLift Implants are permanently placed to lift and hold the enlarged prostate tissues out of the way and increase the opening of the urethra. The permanent implants are delivered through a small needle that comes out of the UroLift delivery device and into the prostate. |
 |
Step 3: The UroLift delivery device s removed, leaving an open urethra designed to provide symptom relief. |
1McVary J Sex Medicine 2014
2Roehrborn J Urology 2013; 2003 AUA Guidelines
3Sonksen J Urology 2016
4Roehrborn Urology Clinics 2016
Videos
Procedure video
Patient testimonials video
Frequently Asked Questions
The UroLift® System is a new minimally invasive treatment designed to treat lower urinary tract symptoms (LUTS) due to benign prostatic hyperplasia (BPH).
The UroLift System consists of a delivery device and tiny permanent implants. FDA cleared in 2013, this unique technology works by directly opening the urethra with tiny implants that hold the enlarged tissue out of the way, like tiebacks on a window curtain. No cutting, heating, or ablating tissue is involved, making the UroLift System the first and only BPH treatment that does not remove prostate tissue and does not negatively impact a man’s sexual function.
The UroLift System is a proven treatment option for BPH patients who are looking for an alternative to drugs or major surgery. You may be considering or scheduled for a TURP/Laser treatment, or are unhappy with or have stopped taking medications. The UroLift System is appropriate for patients seeking a minimally invasive treatment and are concerned about preserving their sexual function and their quality of life.
If you and your doctor decide that the UroLift System treatment is right for you, your doctor will provide the specific, detailed information relating to your condition. In general, the UroLift System is a minimally invasive treatment that entails minimal downtime. Your doctor will use the UroLift delivery device to deploy permanent implants to relieve obstruction caused by the enlarged prostate that is pressing on your urethra. The procedure may be performed under local or general anesthesia and you may be given medication to feel comfortable during the treatment. Typically, no catheter and no overnight stay is required post-treatment.
After the treatment, almost all patients go home the same day without a catheter. There is minimal downtime post-treatment and many patients experience symptom relief in as early as 2 weeks. Patients may experience some urinary discomfort during the recovery period. The most common side effects may include light blood in the urine, some pain or discomfort when urinating, some increased urge to go and discomfort in the pelvis that typically resolve within two to four weeks after the procedure.
Sexual function has been preserved among the hundreds of patients treated in our clinical studies.1,2,3,4 This is a unique benefit of the UroLift System treatment compared with other BPH therapies such as TURP, laser, and even medication.
The UroLift Implant is a permanent implant, and the treatment is intended to be permanent. Durability has been shown to at least 4 years in U.S. clinical data,1 and results will continue to be published as follow-ups continue. One unique aspect of the UroLift System is that it does not preclude retreatment or other BPH treatments, should that be needed and desired in the future.
The implant is made up of standard surgical implantable materials: a nitinol capsular tab, a stainless steel urethral tab, and polyester suture that holds the two tabs together. Your doctor can simply remove the implant, if needed. The suture can be cut and the urethral endpiece can be retrieved with a standard grasper. The capsular tab will remain outside the prostate capsule in place.
The primary contraindications are an obstructive or protruding median lobe of the prostate and a prostate with a volume of >80cc.
Non-clinical testing has demonstrated that the UroLift Implant is MR Conditional. That means that you can be safely scanned in an MR system meeting the following conditions:
- Static magnetic field of 3 Tesla or less
- Maximum spatial gradient magnetic field of 1500 Gauss/cm (15 T/m) or less
- Maximum MR system reported, whole body averaged specific absorption rate (SAR) of 4 W/kg (First Level Controlled Mode)
Under the scan conditions defined above, the UroLift implant is expected to produce a maximum temperature rise of 2.4°C after 15 minutes of continuous scanning.
In non-clinical testing, the image artifact caused by the device extends approximately 15 mm from the UroLift Implant when imaged with a gradient echo pulse sequence and a 3 Tesla MRI system.
Patient implant cards are provided to inform the patient that the UroLift implant is MR Conditional and can safely be scanned only under specific MR conditions.
If you have any questions about MRI safety, please consult your doctor.
No. The implants are placed on the anterior (front) side of the prostate, and a DRE is conducted on the posterior (back) side of the prostate. The implants are not expected to interfere in a DRE.
Over 950 patient-years of clinical data has been presented in peer-reviewed publications to date demonstrating that the UroLift System is safe and effective. Clinical studies have been conducted in the United States, Canada, Europe and Australia.
The first step is to make an appointment with your urologist to determine if you are an appropriate candidate for the treatment. Your physician’s office staff can work with you and your health plan to learn more about your healthcare benefits specific to the UroLift implant procedure.
Yes, all Medicare arriers provide benefits for the UroLift System when medically necessary. Discuss the UroLift System with your physician to determine if the UroLift treatment is an option for you.
A urologist, a doctor who specializes in the treatment of diseases of the urinary system and sex organs, uses the UroLift System to treat urinary symptoms due to BPH. The urologist completes comprehensive training prior to using the UroLift System. Find a UroLift System doctor.
The UroLift System is available for sale in the United States, Europe, Canada and Australia.
NeoTract, Inc. manufactures the UroLift System. The company is based in Pleasanton, California.
- Roehrborn 2016 Urology Clinics
- Roehrborn, 2015 Canadian Journal of Urology, 3-Year Results L.I.F.T. Study
- Roehrborn, 2013 Journal of Urology, L.I.F.T Study
- McVary, 2014 Journal of Sexual Medicine, Preservation of sexual function with the prostatic urethral lift
To learn more, visit urolift.com















